⚡ TL;DR — Sun Poisoning Rash
- A sun poisoning rash — medically called Polymorphous Light Eruption (PMLE) — is an immune reaction to UV exposure, not actual poisoning. It affects up to 15% of people worldwide.
- The rash appears 30 minutes to 2 days after sun exposure as itchy bumps, raised patches, or blisters on sun-exposed skin areas. It resolves without scarring within 10 days.
- UVA rays cause up to 90% of cases — standard sunscreen may not fully protect without broad-spectrum (UVA + UVB) formulas.
- Treatment: protect from further sun, apply hydrocortisone cream, take antihistamines. Severe cases may need phototherapy or prescription corticosteroids.
A sun poisoning rash is one of the most misunderstood skin reactions in warm-weather health. The term “sun poisoning” sounds alarming, but the rash itself — formally known as Polymorphous Light Eruption (PMLE) — is actually an immune system overreaction to UV light, not a toxic event. It’s the most common sun-triggered skin disease worldwide, affecting up to 15% of people according to Cleveland Clinic’s dermatology overview. Understanding what this rash actually is, why it appears, and how to manage and prevent it can significantly improve quality of life for the millions of people affected by it each spring and summer.
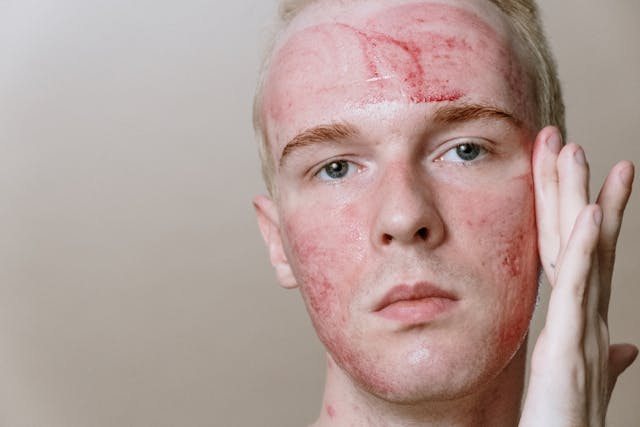
What Is a Sun Poisoning Rash?
A sun poisoning rash refers most precisely to Polymorphous Light Eruption (PMLE) — an immune-mediated skin reaction triggered by UV radiation in people who have developed a sensitivity to sunlight. The term “polymorphous” reflects the fact that the rash looks different in different people (bumps, raised patches, blisters, or hives). The word “eruption” refers to its sudden onset — typically within 30 minutes to several hours of UV exposure, though it can appear up to 2 days later. Mayo Clinic describes PMLE as the most common sun-triggered skin disease, with the rash usually appearing on areas of the body that were covered during winter but exposed as daylight hours lengthen in spring and summer — the upper chest, front of the neck, and forearms are typical locations. Importantly, PMLE resolves on its own within approximately 10 days and does not cause permanent scarring. However, it tends to recur each year, and in some patients worsens over time without treatment.
Symptoms and Appearance
The hallmark symptoms of a sun poisoning rash (PMLE) include: dense clusters of small red bumps; inflamed, raised rough patches of skin; blistering in some cases; intense itching or burning sensation; and, rarely, associated fever and chills in more severe reactions. The rash always appears on sun-exposed areas of the skin — this is an important diagnostic clue distinguishing PMLE from other skin conditions. Because the rash appears on skin that was unexposed to sun over winter, the chest, neck, forearms, and hands are prime targets at the start of the warmer season. As the season progresses and skin gradually “hardens” to UV exposure, the rash tends to become less severe — this natural desensitisation is also the basis for phototherapy treatment.
💡 Did You Know? PMLE affects up to 15% of people worldwide — but it’s far more common in women than men, and more prevalent in people living in higher latitudes where skin gets less year-round UV exposure. It typically first appears in teens and young adults. People of all skin tones can be affected, though it’s reported more commonly in those with lighter skin tones who sunburn easily. Emotional distress from PMLE occurs in over 40% of individuals, according to research cited in medical literature.
What Causes a Sun Poisoning Rash?
The exact mechanism behind a sun poisoning rash is not fully understood. Current evidence suggests that UV radiation alters a compound in the skin, and the immune system mistakenly recognises this altered compound as foreign — mounting an inflammatory response that produces the characteristic rash. Both UVA and UVB light can trigger PMLE, but UVA is responsible for up to 90% of cases, according to Cleveland Clinic. This is clinically important because many older sunscreens primarily protect against UVB (which causes burning) without adequate UVA protection — meaning users could apply sunscreen, avoid burning, and still trigger a PMLE reaction. Only broad-spectrum sunscreens with adequate UVA protection prevent PMLE effectively. Risk factors include being female, having easily sunburning skin, living in high latitudes with lower year-round UV levels, and having a family history of the condition.
How to Treat a Sun Poisoning Rash
The good news about a sun poisoning rash is that most episodes resolve on their own within 10 days without scarring. Treatment focuses on symptom relief and protecting the affected skin from further UV exposure. Immediate steps: get out of the sun and cover the affected area completely. Apply a topical anti-itch cream — products containing at least 1% hydrocortisone (available OTC) can reduce inflammation and itching. Take oral antihistamines to manage the allergic-type response. Cool compresses can provide comfort to inflamed areas. Avoid picking or scratching the rash. For moderate cases, Mayo Clinic recommends applying OTC hydrocortisone cream and notes that doctors may prescribe topical corticosteroids for more significant outbreaks. For severe or persistent PMLE, doctors may prescribe: stronger prescription corticosteroids (oral or topical); antimalarial medications like hydroxychloroquine in recalcitrant cases; or phototherapy (controlled UV exposure) as a desensitisation protocol — repeated, graduated UV exposure teaches the skin to tolerate sunlight without reacting. For broader guidance on sun skin reactions, see our sun poisoning guide and sun poisoning vs sunburn comparison.

Preventing Future Sun Poisoning Rash Outbreaks
Prevention of sun poisoning rash outbreaks requires a layered sun protection strategy. Always use broad-spectrum SPF 30+ sunscreen — applied 15 minutes before outdoor exposure and reapplied every 2 hours and after water contact. The “broad spectrum” labelling is essential — it ensures UVA protection, which is what primarily triggers PMLE. Wear protective UPF-rated clothing that covers areas prone to PMLE reactions (upper chest, forearms, back of hands). Avoid peak sun hours (10am–2pm) in the first weeks of the warmer season, when skin is most sensitive after winter. Gradually increase sun exposure as the season progresses to allow natural desensitisation. Some clinicians recommend a short course of prophylactic phototherapy at the start of each spring for people with severe recurrent PMLE — this “hardens” the skin before natural season-onset exposure begins. Beta-carotene supplements have been used historically for PMLE prevention, though evidence is modest. If you know you’re prone to sun poisoning rash, speak to a dermatologist before summer about whether prophylactic phototherapy or prescription prevention is appropriate for you.
When to See a Doctor for Sun Poisoning Rash
See your doctor for a sun poisoning rash if: the rash is widespread, painful, or severely blistered; it’s accompanied by significant fever or chills; it does not improve within 10 days of sun avoidance; it occurs repeatedly and is disrupting your quality of life; or you’re unsure whether the rash is PMLE or something else — other conditions including lupus, drug photosensitivity reactions, and contact dermatitis can cause sun-triggered rashes that look similar. As Mayo Clinic notes, PMLE rashes look similar to rashes caused by other diseases, some of which are serious — making prompt diagnosis important when a sun-triggered rash appears unexpectedly. A dermatologist can confirm PMLE through clinical history, phototesting, or skin biopsy in uncertain cases. Seek immediate medical care if the rash is widespread, extremely painful, associated with high fever, or accompanied by breathing difficulty (possible anaphylaxis, though rare).
☀️ A sun poisoning rash is your immune system overreacting to UV — not actual poisoning.
It resolves within 10 days, doesn’t scar, and is highly preventable with broad-spectrum SPF and protective clothing. See a dermatologist if it recurs each year — phototherapy can significantly reduce future outbreaks.
Disclaimer: This article is for educational purposes only. If you have a rash with no obvious cause, see your healthcare provider for diagnosis and treatment, as rashes from different causes can look similar.

